
He cholesterol and the high blood pressure are the only ones enemies of the heart. A large study showed other underestimated factors that also accelerate the cardiac aging silently, linked to the psychosocial stress.
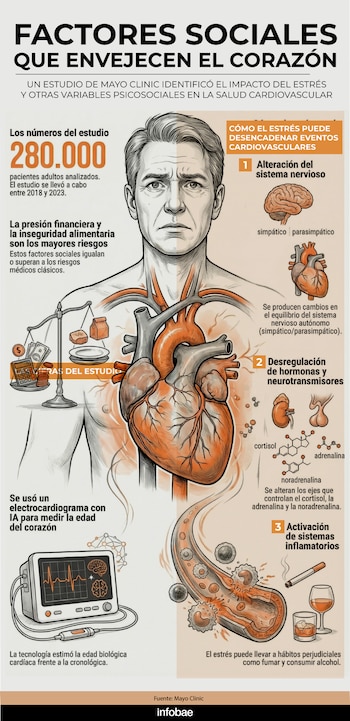
The research, led by doctor Amir Lerman of the Department of Cardiovascular Medicine of the Mayo Clinic in Rochester, United States, analyzed more than 280,000 adult patients between 2018 and 2023, and highlighted the importance of the so-called social determinants of health (SDH).
The study, published in Mayo Clinic Procedurespointed to the financial pressure and the food concernunderstood as the impossibility of meeting nutritional needs, as the social determinants that most increase the risk cardiovascular.
In increasingly long-lived societiesthe expectation is no longer just to live longer, but to achieve a better quality of life during that extended period. This new scenario requires the development of innovative strategies and advanced early detection and prevention methods.

The work evaluated the participants through a questionnaire that covered 9 social aspects: stress, physical activity, social connection, housing, economic pressure, food insecuritytransportation, nutrition and education needs.
The study found that, among social determinants of health (SDH)the financial pressure and food insecurity were the most important determinants.
The biological age of the heart was estimated using a electrocardiogram algorithm assisted by artificial intelligence (AI-ECG), which allowed us to calculate the difference between the person’s chronological age and heart age dear.
a major lag in this index indicates that the heart ages faster than the rest of the organism, which increases the risk of future cardiovascular deterioration. The algorithm, validated by Mayo Clinic researchers, proved to be an innovative and non-invasive technique capable of detecting risk factors not identified in routine medical check-ups.
In the world, the cardiovascular disease is still the main cause of mortality and morbiditydespite preventive strategies and scientific advances.
The incidence of cardiovascular disease increases markedly with age and there are growing inequities in burden and mortality between different sex and race groups, which could be because preventive efforts are largely focused on traditional risk factors and not in the social conditions in which people are born, live, work and learnknown as social determinants of health (SDH).

As cardiologist Martín Lombardero explained in Infobae“cardiovascular clinical practice often overlooks the impact of mental health and the importance of its inclusion in cardiovascular care; This must change.” The specialist highlighted that the new clinical consensus published this year by the European Society of Cardiology (ESC) highlights the role of psychological stress in cardiovascular risk.
“There is talk of psychosocial stress as the main protagonist of chronic stress. The ESC Consensus defines psychosocial stress when an individual perceives and responds “badly” to a social demand (family problems, social isolation, financial pressures and work) because it exceeds its ability to adapt or exceeds the body’s “metabolic” tolerance range to be able to face that demand,” Lombardero explained.
The psychic alterations interact with cardiovascular health in ways bidirectional, Lombardero specified:“Psychological stress affects the heart, but at the same time, a cardiological disease affects our mind.”

Among all the social aspects evaluated, the financial pressure and the concern about food stood out as the factors with the greatest impact on heart aging.
Both the economic uncertainty —like the permanent worry about making ends meet—like the inability to maintain a sufficient and balanced diet They exert a direct effect, accelerating biological cardiac deterioration in different groups of the population, both men and women.
Furthermore, other factors such as housing problems and physical inactivity (sedentary lifestyle) were identified as robust predictors of mortality, sometimes equaling or exceeding conventional risks.
The traditional paradigm, focused on high cholesterol and hypertension as the main cardiovascular risk factors, is altered by these results. According to both means, the statistical analysis of the sample revealed that the social determinants of healthespecially the financial pressure and the food insecurityequal or exceed the predictive capacity of classical medical factors on cardiac aging and mortality.
Given these findings, the research led by Dr. Lerman insists on the need to strengthen cardiological prevention through active inclusion of social evaluation in medical consultation. In the specialist’s words, “there are social factors that we do not identify or investigate in our patients and that could reverse biological aging.”

Early identification of these risks would allow for the design of more effective and personalized preventive strategies, as well as enhance truly patient-centered care.
However, the authors cautioned that the majority of patients studied identified as non-Hispanic white, so the study results may not accurately apply to other specific populations and racial/ethnic groups. Furthermore, the artificial intelligence algorithm used was specifically validated in the Mayo Clinic setting, so caution is required when extrapolating these data internationally.
It can do so due to several factors and they can act all at once, Lombardero pointed out and highlighted:
- The changes in the sympathetic/parasympathetic balance: that is, changes in the control of the autonomic nervous system.
- The alteration of axles that control hormones and neurotransmitters: like cortisol, adrenaline, norepinephrine inter alia.
- By activation of the systems inflammatory: stress can also lead to acquiring unhealthy habitsas smoke and consume alcohol.

